November is Diabetes Awareness Month. The diabetes that most are aware of, I think, is Type 2 Diabetes. This is good, I suppose, as the condition has grown to epidemic proportions.
More people are unaware that Type 1 has also increased with great regularity. This condition afflicts children, as well as adult onset victims, but what exactly is the difference? Type 1 is in no way connected to weight or “bad sugar” and diet behavior. It can also not be controlled, except with the use of insulin.
As I was diagnosed after a bad case of childhood flu, I’d still say perhaps some Type 1 is caused by a virus. I’ve met many who’d swear to that and I put myself in that category, not that I was ever listened to as an adolescent. At any rate, it’s hard for me to be certain of how I feel about “awareness.”
During most of my lifetime, I have not given myself shots in front of people. Some today actually consider this an unhealthy attitude, but I was extremely self-conscious about being different, and so medication became, to me, a very private matter. I was a proud adolescent, and I simply memorized the diagrams in the “shot brochures,” the ones picturing the body with certain sections shaded as suitable for injection and absorption. The upper arms and thighs, the hips, and even the stomach are all “fair game.” The diabetic is also told to vary the injection site, to space the injections out say across the leg or down the leg, and then, the child should perhaps move to the other leg.
I’m almost sure I gave my first shot in my thigh since that site had been mentioned and re-mentioned in the literature. Also, when I’d tried to inject my upper arm with the opposite hand, I’d found the reaching over myself much more difficult than one would imagine, perhaps due to my short arms. However, I could reach my youthful, then “good-looking” legs–the same legs I wanted to look good when I wore a swimsuit or shorts, or whenever I sported whatever tan I could muster. No matter what healthcare professionals swore, my blunt needles left marks. I had “tracks,” I thought. At times, I suffered bruising.
I went to college during an age when drugs were turning up everywhere. I was once at what I had been told was a “fun party.” We were out on a farm “off campus,” so many young people getting to know each other, talking under the stars. No it was not Woodstock and no one was naked. Everyone was just generally having a good time. Then the human “stars” arrived, a couple from a popular bar downtown. No names are in my memory, not even clear faces. Just a medium built, muscled guy, with shoulder-length hair, and he walked with a silver-balled cane. I have no idea why he was “the star.” He was wearing spats. The girl, of course, had long flowing hair.
I do remember a while later, in the haze of moonlight, that I climbed a ladder to get on top of the garage. Not one of my usual activities, but I guess I was trying to be “wild” by joining the group that had moved up there. What I saw on the flat roof was the same man getting ready to “shoot up.” What I did was climb back down. The stars reeled overhead. I told those right behind me on the rungs that I was going to be sick, and the way down cleared.
How could anyone do that? This was my only thought. Why would anyone do that willingly to one’s body? Not that any of the party-goers or “cool people” knew then or probably know now much about diabetes. Let’s hope they learned more about life and are still living it. I have no other memories of the night, except that I think I looked for my closer friends again and left soon thereafter. Maybe T1D saved me from the hippie drug scene (nothing compared to the drug scene now). Or maybe just a good upbringing and common sense. I always felt I had to know about what time it was. No losing track of consciousness.
At any rate, insulin pens and the insulin pump have changed and lessened the pain of taking insulin these days. The pump and glucose monitors are not yet, though, totally automatic. The diabetic child/teen or a parent still has to be on top of blood sugar levels, dosages, diet and the like. Believe it or not, a phone app is now helping!
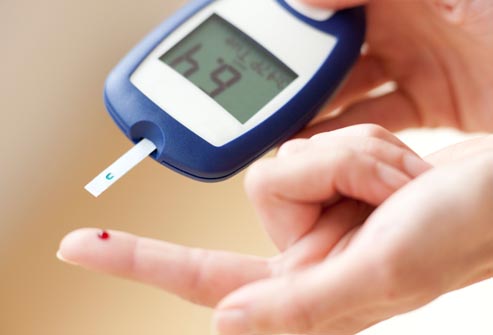
Until the continuous glucose monitors can become 100 percent effective, public blood testing using the finger or arm seems to be more the subject of controversy. And these days, lows not highs are the concern. Most schools have now been effectively prevailed upon to let children blood test right in class, say if they are feeling low and/or if they feel the need to make sure they’re all right before a test. Of course, this was never even a possibility for me when growing up, not that I would have consented to do so really.
Besides the fact that I did not want to be stared at as a diabetic while growing up, I think it’s my Southern upbringing—who would test their blood sugar in front of others sitting down to eat? No, doesn’t sound appetizing—of course, I would never deny someone the right. Still—after ordering at a restaurant, what’s wrong with excusing one’s self to the restroom? If you use an insulin pump at the table, most just think you’re looking at a phone if they even notice. Not that people didn’t or don’t know I’m a diabetic
These days, if in a crowd of busy people, I do perhaps just turn away on an airport bench to test my blood—still, as I was involved professionally in a more business-like atmosphere, hard to imagine the business lunch, sales meeting, work meeting in which I would have thought it socially acceptable to squeeze blood from my finger. Actually, the reason I’m for diabetic awareness is that a cure or more effective methods of treatment seem so close.
Life could be so much easier for the kids coming up. Many are intrigued by the idea of “smart insulin.” This is a dosage that would have to be taken in the morning each day—and then supposedly, the insulin reacts chemically with various levels of glucose throughout the day automatically. We’re back to one shot a day! Not sure about the blood testing.
My favorite so far is the discovery/manufacture of beta cells by Harvard professors. This is touted as a cure, though actually it seems to be simply a very much improved treatment of T1D. The encapsulated beta cells are in some sort of bandaid-size implement that can be inserted into the backside of the diabetic every two-three years, and these cells then work much the same way as the cells within a normal pancreas. Again, not sure how the glucose testing would still go, but seems like it would eliminate the needs of injections and the like?
The reason to be involved in diabetic awareness now is that there is hope. Actual hope that healthcare can not only keep a child alive, but the very real idea that healthcare—rather than leading to only more healthcare—will one day actually be able to provide cures for various diseases, diabetes among them. Yes, if one tests positive for the possibility of developing T1D these days (remember all those tales of inherited tendencies)—tests are now being run on possible vaccines. Could the ravages of that virus have been stopped in my once supposedly pre-disposed body? Maybe now, or maybe soon!
I have survived a lifetime with T1D by not letting myself even consider life another way. Yes, best to live and make the best of what I had, not pine for a future that could not be mine. I still don’t pine really—I’m 65 years old, and I find a way to do what I need or want to do (now that the need for health insurance no longer binds me). I do now, however, seek to touch the future—for the younger people, could not life be made better, more affordable, less of a burden or a pain to the body? That’s what I think diabetic awareness can lead us to: touching the future.
All together now, no resigning ourselves. Healthcare is good, but how about freedom from such involved healthcare on a daily basis or how about a cure? Let’s touch the future.